Happy Monday!
Most people think of TB-500 as strictly a peptide for healing injuries, and rightfully so.
However, a new study just dropped in International Immunopharmacology that examines TB-500 through the lens of brain function.
And the results are worth your time.
Today, I’ll break down what this research team actually did, what they found, how the peptide appears to be working inside the brain, and what this could mean for the future of Alzheimer’s research.
The Study
The researchers in this study tested two fragments of thymosin beta-4. The first is TB-500. That's the actin-binding fragment most of you know.
The second is Ac-SDKP. That's a smaller fragment from the other end of the thymosin beta-4 molecule. It's known mostly for its anti-inflammatory and anti-fibrotic activity.
Full-length Tβ4 is a relatively large peptide at nearly 5,000 daltons. That size makes it harder to cross the blood-brain barrier. TB-500 and Ac-SDKP are much smaller. The thinking was that these fragments might actually reach the brain more effectively than the parent molecule.
They tested both fragments in lab-grown brain cells and in living mice with Alzheimer's-like disease.
The Brain Cell Test
The team started with two types of brain cells.
First, they used HT22 cells and primary cortical neurons.
These are brain cells that can be grown in a dish. They exposed these cells to amyloid-beta (Aβ), which is the toxic protein fragment that builds up in Alzheimer's brains and kills neurons. Then they treated the cells with TB-500 and Ac-SDKP to determine whether the peptides could protect them.
Second, they used BV2 microglia.
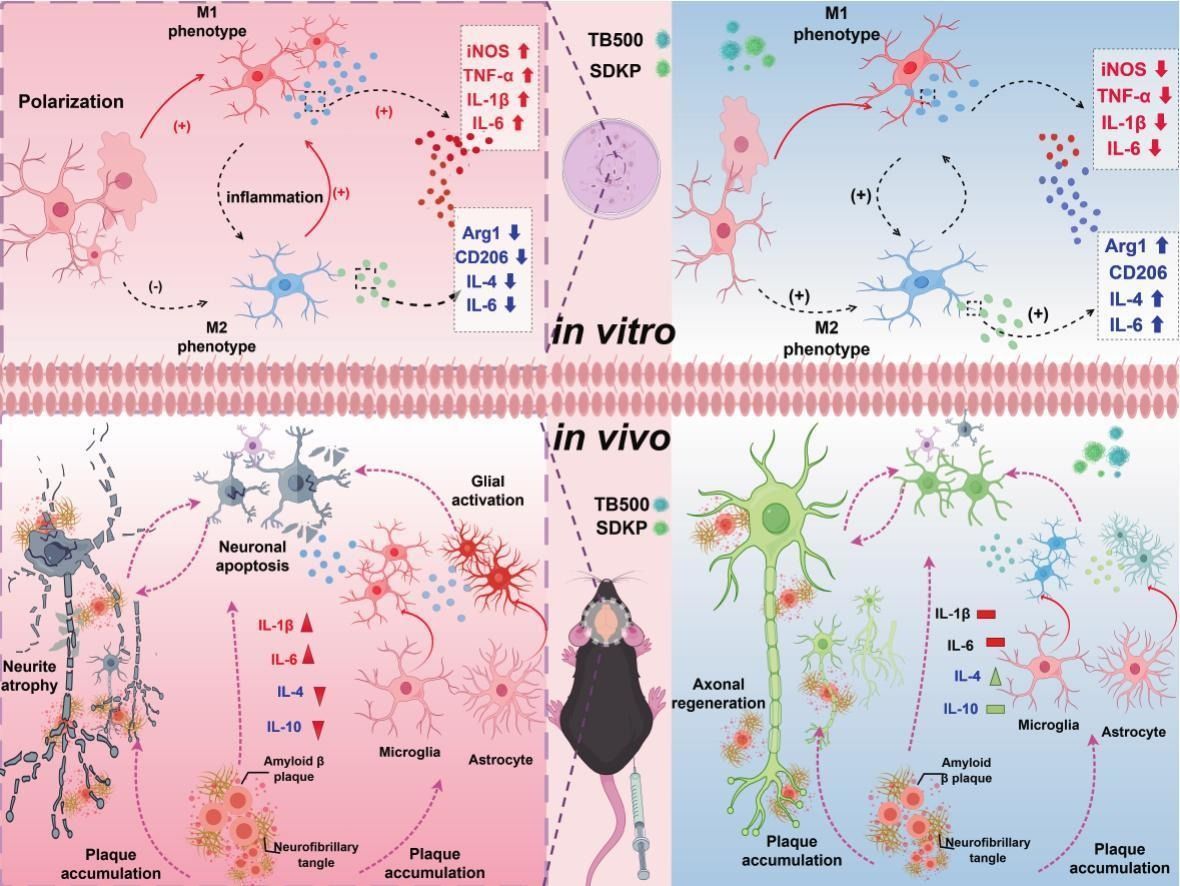
Microglia are the brain's resident immune cells. In a healthy brain, they clean up debris and protect neurons. In Alzheimer's, they get stuck in an aggressive, inflammatory state called M1 polarization.
When microglia go M1, they release inflammatory chemicals that damage the neurons around them.
The researchers activated these microglia with LPS (a bacterial toxin that triggers inflammation) and then tested whether the peptides could calm them down.
The Results
In the neurons exposed to amyloid-beta, both TB-500 and Ac-SDKP did three things.
They protected cell viability. Fewer neurons died when the peptides were present.
They reduced the expression of genes linked to programmed cell death (apoptosis).
They rescued neurite atrophy. Neurites are the branch-like extensions that neurons use to communicate with each other. When neurites shrink, the brain's communication network breaks down. That's a major driver of cognitive decline in Alzheimer's. Both peptides helped preserve those connections.
In the microglia experiments, the results were just as clear.
Both TB-500 and Ac-SDKP suppressed nitric oxide production, a marker of inflammatory activation. They reduced the expression of pro-inflammatory cytokines. And they blocked M1 microglial polarization.
In plain terms, the peptides helped shift the brain's immune cells from "attack mode" back toward a calmer, less destructive state.
The Mice Test
The team also used TB-500 and Ac-SDKP in 5xFAD mice.
This is one of the most aggressive Alzheimer's mouse models available. These mice carry five different mutations linked to familial Alzheimer's disease. They develop amyloid plaques early. They show neuroinflammation. They lose cognitive function.
The researchers treated these mice with TB-500 and Ac-SDKP and then ran two gold-standard behavioral tests.
The Morris water maze is a fun way to test how well mice can learn and remember spatial tasks. In this test, mice are placed in a pool of water and need to find a hidden platform to escape.
Mice with Alzheimer's-like symptoms often take a bit longer and make more mistakes, which helps researchers understand their memory challenges.
The novel object recognition test is another interesting test that assesses whether a mouse can tell the difference between something it has seen before and something new, and it also relies on working memory.
These tests provide valuable insights into how memory works in mice and can help us better understand memory issues, such as those seen in Alzheimer's disease.
What They Found
The treated mice performed significantly better on both tests.
In the Morris water maze, mice that received TB-500 or Ac-SDKP found the platform faster and more efficiently than untreated 5xFAD mice.
In the novel object recognition test, treated mice showed better ability to distinguish new objects from familiar ones. Their memory was measurably improved.
Then the researchers examined what was happening in the brains of these mice.
Analysis showed that glial activation was markedly reduced in treated mice. That means microglia and astrocytes were less inflamed. Neuronal apoptosis was also reduced. Fewer brain cells were dying.
The peptides also restored axonal density in the perirhinal cortex. The perirhinal cortex is a brain region involved in object recognition and memory.
In Alzheimer's disease, the nerve fibers in this area degenerate. TB-500 and Ac-SDKP appeared to help preserve or rebuild those fibers.
The Amyloid Plaque Question
Interestingly, the peptides did NOT reduce the overall amyloid plaque burden in the hippocampus.
The plaques were still there. But the mice still got better. Their memory improved. Their neurons survived at higher rates. Their inflammation went down. Their axonal connections were preserved.
This is a significant finding. It challenges the idea that you have to clear amyloid plaques to improve Alzheimer's outcomes.
The authors specifically note that their results "challenge the Aβ-centric therapeutic paradigm." The peptides worked by making the brain more resilient to the damage plaques cause, rather than by removing the plaques themselves.
What This Means for the Future
This is the first study I've seen that directly tests TB-500, the actual synthetic fragment, in a rigorous Alzheimer's model. Not just the full-length thymosin beta-4.
The fact that both TB-500 and Ac-SDKP improved memory in 5xFAD mice without clearing amyloid plaques opens a fundamentally different therapeutic conversation.
It suggests that neuronal resilience and inflammation control might matter more than plaque removal. That idea has been building across the neurology field, and this study adds real weight to it.
The authors themselves note several areas that still need work.
Blood-brain barrier penetration needs to be directly measured for both fragments.
Direct neuronal targets need further identification. And they flag that sex-dependent responses need to be studied, since AD affects men and women differently.
Final Thoughts
This is early-stage research, but it's well-designed.
The fact that TB500 and Ac-SDKP improved cognitive outcomes, reduced neuroinflammation, preserved axonal density, and protected neurons from death, all without reducing plaque burden, is a genuinely important finding.
It won't change clinical practice tomorrow, but it should change the conversation about where peptide research is headed.
The next time you go to load up some TB-500, know that you are doing your brain a world of good!
Best,
Hunter Williams
Source:
Ou H, Chen R, Zhou L, Zhang Y, Zhao S, Yang Z. "Thymosin β4-derived peptides alleviate neuroinflammation and neurite atrophy in both in vitro models and in vivo 5×FAD mice: A potential therapy for memory improvement in Alzheimer's disease." International Immunopharmacology. 2025. doi: 10.1016/j.intimp.2025.116097.